 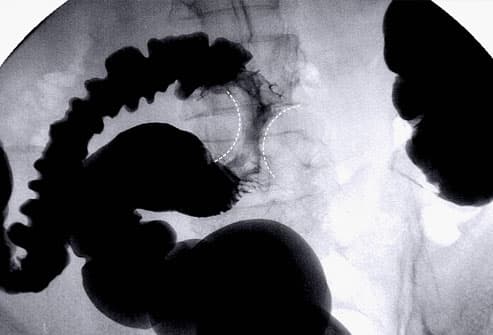
Diverticular disease. DIVERTICULAR DISEASE OVERVIEWA diverticulum is a pouch- like structure that can form through points of weakness in the muscular wall of the colon (ie, at points where blood vessels pass through the wall) (figure 1). Diverticulosis affects men and women equally. The risk of diverticular disease increases with age. It occurs throughout the world but is seen more commonly in developed countries. WHAT IS DIVERTICULAR DISEASE? Diverticulosis — Diverticulosis merely describes the presence of diverticula. Diverticulosis is often found during a test done for other reasons, such as flexible sigmoidoscopy, colonoscopy, or barium enema. Most people with diverticulosis have no symptoms and will remain symptom free for the rest of their lives. This may be caused by increased pressure within the colon or by hardened particles of stool, which can become lodged within the diverticulum. The symptoms of diverticulitis depend upon the degree of inflammation present. The most common symptom is pain in the left lower abdomen. Other symptoms can include nausea and vomiting, constipation, diarrhea, and urinary symptoms such as pain or burning when urinating or the frequent need to urinate. Diverticulitis is divided into simple and complicated forms. Complications associated with diverticulitis can include the following. In approximately 5.
Is bleeding with a bowel movement normal? Anyone who sees blood after a bowel movement should consult with their healthcare provider to determine if further testing or evaluation is needed. This is an older test and has been largely replaced by computed tomography (CT) scan. 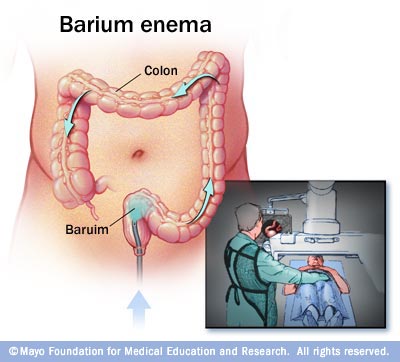
If diverticulitis (not just diverticulosis) is suspected, the above three tests should not be used because of the risk of perforation. TREATMENTDiverticulosis — People with diverticulosis who do not have symptoms do not require treatment. Barium Enema X Ray Versus Colonoscopy Diet 5However, most clinicians recommend increasing fiber in the diet, which can help to bulk the stools and possibly prevent the development of new diverticula, diverticulitis, or diverticular bleeding. Fiber is not proven to prevent these conditions in all patients but may help to control recurrent episodes in some. Increase fiber — Fruits and vegetables are a good source of fiber (table 1). The fiber content of packaged foods can be calculated by reading the nutrition label (figure 2). However, this belief is completely unproven. We do not suggest that patients with diverticulosis avoid seeds, corn, or nuts. Diverticulitis — Treatment of diverticulitis depends upon how severe your symptoms are. Home treatment — If you have mild symptoms of diverticulitis (mild abdominal pain, usually left lower abdomen), you can be treated at home with a clear liquid diet and oral antibiotics. However, if you develop one or more of the following signs or symptoms, you should seek immediate medical attention. During this time, you are not allowed to eat or drink; antibiotics and fluids are given into a vein. If you develop an abscess of the colon, you may require drainage of the abscess (usually performed by placing a drainage tube across the abdominal wall) or by surgically opening the affected area. Surgery — If you develop a generalized infection in the abdomen (peritonitis), you will usually require an emergency operation. A two- part operation may be necessary in some cases. A colostomy is an opening between the colon and the skin, where a bag is attached to collect waste from the intestine. The lower end of the colon is temporarily sewed closed to allow it to heal (figure 3). 
Answer questions and earn CME/CNE. Each year, the American Cancer Society (ACS) publishes a summary of its guidelines for early cancer detection along with. Irritable Bowel Syndrome Definition Irritable bowel syndrome (IBS) is a common intestinal condition characterized by abdominal pain and cramps; changes in bowel. You are then able to empty your bowels through the rectum. Sometimes patients require up to a year to recover from the first operation, depending on how sick they were. In non- emergency situations, the diseased area of the colon can be removed and the two ends of the colon can be reconnected in one operation, without the need for a colostomy. Surgery versus medical therapy — An operation to remove the diseased area of the colon may not be necessary if you improve with medical therapy. However, people who are treated with an operation are felt to be cured, since only 1. Thus, surgery may be recommended for people with repeated attacks of diverticulitis or if there are severe or repeated episodes of bleeding. The decision depends in part upon your other medical conditions and ability to undergo surgery. Some healthcare providers recommend surgery after the first attack of diverticulitis in people who are less than 4. The reason for this is that the disease may be more severe in this age group and there may be an increased risk of recurrent disease that will ultimately require surgery. Thus, having surgery at a young age could potentially eliminate the chances of developing worsened disease. The decision to undergo surgery ultimately depends upon your surgeon's recommendations. In many cases, an elective operation can be performed laparoscopically, using small incisions, rather than the typical vertical (up and down) abdominal incision. Laparoscopic surgery usually allows you to recover more quickly and shortens the hospital stay. After diverticulitis resolves — After an episode of diverticulitis resolves, if you have not had a recent colonoscopy, the entire length of the colon should be evaluated to determine the extent of disease and to rule out the presence of abnormal lesions such as polyps or cancer. Recommended tests include colonoscopy, barium enema and sigmoidoscopy, or CT colonography. However, some people will need further testing or treatment to stop bleeding, which may include a colonoscopy, angiography (a treatment that blocks off the bleeding artery), bleeding scan, or surgery. DIVERTICULAR DISEASE PROGNOSISDiverticulosis — Over time, diverticulosis may cause no problems or it may cause episodes of bleeding and/or diverticulitis. Approximately 1. 5 to 2. Diverticulitis — Approximately 8. After successful treatment for a first attack of diverticulitis, one- third of patients will remain asymptomatic, one- third will have episodic cramps without diverticulitis, and one- third will go on to have a second attack of diverticulitis. The prognosis tends to remain similar following a second attack of diverticulitis. Only 1. 0 percent of people remain symptom- free after a second attack. Subsequent attacks tend to be of similar severity, not increasing in severity as previously believed. WHERE TO GET MORE INFORMATIONYour healthcare provider is the best source of information for questions and concerns related to your medical problem. This article will be updated as needed on our website (www. Related topics for patients, as well as selected articles written for healthcare professionals, are also available. Some of the most relevant are listed below. Patient level information — Up. To. Date offers two types of patient education materials. The Basics — The Basics patient education pieces answer the four or five key questions a patient might have about a given condition. These articles are best for patients who want a general overview and who prefer short, easy- to- read materials. Patient education: Diverticulitis (The Basics)Beyond the Basics — Beyond the Basics patient education pieces are longer, more sophisticated, and more detailed. These articles are best for patients who want in- depth information and are comfortable with some medical jargon. Patient education: Blood in the stool (rectal bleeding) in adults (Beyond the Basics)Patient education: Flexible sigmoidoscopy (Beyond the Basics)Patient education: Colonoscopy (Beyond the Basics)Patient education: High- fiber diet (Beyond the Basics)Patient education: Colon and rectal cancer screening (Beyond the Basics)Professional level information — Professional level articles are designed to keep doctors and other health professionals up- to- date on the latest medical findings. These articles are thorough, long, and complex, and they contain multiple references to the research on which they are based. Professional level articles are best for people who are comfortable with a lot of medical terminology and who want to read the same materials their doctors are reading. Acute diverticulitis complicated by fistula formation. Clinical manifestations and diagnosis of acute diverticulitis in adults. Colonic diverticular bleeding. Segmental colitis associated with diverticulosis. Colonic diverticulosis and diverticular disease: Epidemiology, risk factors, and pathogenesis. Acute colonic diverticulitis: Medical management. The following organizations also provide reliable health information. Our peer review process typically takes one to six weeks depending on the issue. Cholecystectomy - Wikipedia. Laparoscopic Cholecystectomy as seen through laparoscope. Cholecystectomy (; plural: cholecystectomies) is the surgical removal of the gallbladder. It is a common treatment of symptomatic gallstones and other gallbladder conditions. Surgical options include the standard procedure, called laparoscopic cholecystectomy, and an older, more invasive procedure, called open cholecystectomy. The surgery can lead to postcholecystectomy syndrome. Indications. Risk factors for gall bladder cancer include a . This is because open surgery leaves the patient more prone to infection. The camera illuminates the surgical field and sends a magnified image from inside the body to a video monitor, giving the surgeon a close- up view of the organs and tissues. The surgeon watches the monitor and performs the operation by manipulating the surgical instruments through the operating ports. To begin the operation, the patient is placed in the supine position on the operating table and anesthetized. A scalpel is used to make a small incision at the umbilicus. Using either a Veress needle or Hasson technique, the abdominal cavity is entered. The surgeon inflates the abdominal cavity with carbon dioxide to create a working space. The camera is placed through the umbilical port and the abdominal cavity is inspected. Additional ports are opened inferior to the ribs at the epigastric, midclavicular, and anterior axillary positions. The gallbladder fundus is identified, grasped, and retracted superiorly. With a second grasper, the gallbladder infundibulum is retracted laterally to expose and open Calot's Triangle (cystic artery, cystic duct, and common hepatic duct). The triangle is gently dissected to clear the peritoneal covering and obtain a view of the underlying structures. The cystic duct and the cystic artery are identified, clipped with tiny titanium clips and cut. Then the gallbladder is dissected away from the liver bed and removed through one of the ports. This type of surgery requires meticulous surgical skill, but in straightforward cases, it can be done in about an hour. Recently, new techniques have been developed to perform this surgery through a single incision in the patient's umbilicus. This advanced technique is called Laparoendoscopic Single Site Surgery or . In this procedure, instead of making 3- 4 four small different cuts (incisions), a single cut (incision) is made through the navel (umbilicus). Through this cut, specialized rotaculating instruments (straight instruments which can be bent once inside the abdomen) are inserted to do the operation. The advantage of LESS / SILS operation is that the number of cuts is further reduced to one and this cut is also not visible after the operation is done as it is hidden inside the navel. A meta- analysis published by Pankaj Garg et al. Failure of this technique is common as a consequence of large or impacted common bile duct (CBD) stones. A new technique, LABEL (Laser- Assisted Bile duct Exploration by Laparoendoscopy) has been developed to enhance LBDE in cases of impacted or large stones using holmium- laser increasing the feasibility of the transcystic stone retrieval and reducing overall operative time in the treatment of choledocholithiasis. In open cholecystectomy, a surgical incision of approximately 1. The liver is retracted superiorly, and a top- down approach is taken (from the fundus towards the neck) to remove the gallbladder from the liver, typically using electrocautery. Surgical incision points are highlighted; the one at top right is barely visible. The gall bladder was removed via the incision at the navel. There is a fourth incision (not shown) on the patient's right lower flank, used for draining. All incisions have healed well and the most visible remaining effect of surgery is from the pre- operative hair removal. The 3 abdominal incisions are approximately 6mm, while the fourth incision near the umbilicus is 1. Minor inflammation can be seen surrounding each site due to skin irritation caused by removal of Tegaderm dressings. Laparoscopic cholecystectomy does not require the abdominal muscles to be cut, resulting in less pain, quicker healing, improved cosmetic results, and fewer complications such as infection and adhesions. Most patients can be discharged on the same or following day as the surgery, and can return to any type of occupation in about a week. An uncommon but potentially serious complication is injury to the common bile duct, which connects the cystic and common hepatic ducts to the duodenum. An injured bile duct can leak bile and cause a painful and potentially dangerous infection. Many cases of minor injury to the common bile duct can be managed non- surgically. Major injury to the bile duct, however, is a very serious problem and may require corrective surgery. This surgery should be performed by an experienced biliary surgeon. Adhesions and gangrene can be serious, but converting to open surgery does not equate to a complication. A Consensus Development Conference panel, convened by the National Institutes of Health in September 1. The panel noted, however, that laparoscopic cholecystectomy should be performed only by experienced surgeons and only on patients who have symptoms of gallstones. In addition, the panel noted that the outcome of laparoscopic cholecystectomy is greatly influenced by the training, experience, skill, and judgment of the surgeon performing the procedure. Therefore, the panel recommended that strict guidelines be developed for training and granting credentials in laparoscopic surgery, determining competence, and monitoring quality. According to the panel, efforts should continue toward developing a noninvasive approach to gallstone treatment that will not only eliminate existing stones, but also prevent their formation or recurrence. One common complication of cholecystectomy is inadvertent injury to analogous bile ducts known as Ducts of Luschka, occurring in 3. It is non- problematic until the gall bladder is removed, and the tiny supravesicular ducts may be incompletely cauterized or remain unobserved, leading to biliary leak post- operatively. The patient will develop biliary peritonitis within 5 to 7 days following surgery, and will require a temporary biliary stent. It is important that the clinician recognize the possibility of bile peritonitis early and confirm diagnosis via HIDA scan to lower morbidity rate. Aggressive pain management and antibiotic therapy should be initiated as soon as diagnosed. During laparoscopic cholecystectomy, gallbladder perforation can occur due to excessive traction during retraction or during dissection from the liver bed. It can also occur during extraction from the abdomen. Infected bile, pigment gallstones, male gender, advanced age, perihepatic location of spilled gallstones, more than 1. Spilled gallstones can be a diagnostic challenge and can cause significant morbidity to the patient. Clear documentation of spillage and explanation to the patient is of utmost importance, as this will enable prompt recognition and treatment of any complications. Prevention of spillage is the best policy. If cancer is present, a reoperation to remove part of the liver and lymph nodes will be required in most cases. The cause is unclear, but is presumed to involve the disturbance to the bile system. Most cases clear up within weeks or a few months, though in rare cases the condition may last for many years. It can be controlled with medication such as cholestyramine. This occurs in about 0. Open and laparoscopic surgeries have essentially equal rate of injuries, but the recent trend is towards fewer injuries with laparoscopy. It may be that the open cases often result because the gallbladder is too difficult or risky to remove with laparoscopy)abscesswound infectionbleeding (liver surface and cystic artery are most common sites)herniaorgan injury (intestine and liver are at highest risk, especially if the gallbladder has become adherent/scarred to other organs due to inflammation (e. Good hydration and hygiene (water and fruit juice; using stool softener if prescribed; brushing teeth gently; and taking a light shower and changing bandages about 4. This probably would differ for an open or complicated procedure, and possibly among facilities. Postoperative cystic duct stump leaks. It was rarely reported in open cholecystectomy patients. Since the advent of laparoscopic cholecystectomy the incidence of CDSL has increased with one study indicating that it occurs in 0. Cystic duct displacement: 1a. Improper firing can cause the clip to displace as one study showed clipless cystic ducts after placement of 2 cystic duct clips. Cystic duct displacement could be due to abnormal cystic duct morphological features. This could place constrictions which thus could lead to improper firing. A solution is to suture the duct or as last resort leave a T tube or Jackson- pratt drain intraoperatively. Necrosis of cystic duct stump proximal to clip: This would occur proximal to the applied clip. Necrosis may be secondary to electrocautery creating a phenomenon called . Ischemic necrosis secondary to devascularization: One study showed that blood flow can be disrupted from dissecting. One study showed a pseudoaneurysm of the right hepatic artery causing vascular disrupting blood supply to the cystic duct. A solution is dividing the cystic artery distally. Increased biliary pressure: This can be due to a retained common bile duct stone creating pressure in the biliary tree. This may be the most rare causes of CDSL. High WBC is described in 6. Liver function tests can be highly variable. Computed tomography has a high sensitivity approaching 1. The most successful imaging is from ERCP. ERCP has the additional value of allowing for treatment which often consists of sphincterotomy with common bile duct stenting. With endoscopic drainage, CDSLs often resolve without the need for reoperation. Epidemiology. 1. 01. Goldman, Lee (2. 01. Goldman's Cecil Medicine (2.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
